Guest post by:*
Heather Burgess
Epidemiologist, Overdose Surveillance, BCCDC
Heather Palis
Post-Doctoral Fellow, Provincial Overdose Cohort , BCCDC
*Supplemental contributors recognized at the bottom.
In 2016, British Columbia (BC) declared a public health emergency in response to rapidly rising drug overdose deaths. More than four years later, the public health emergency continues as the province responds to a second public health emergency: the COVID-19 pandemic.
Prior to COVID-19, overdose deaths in BC were declining, even as rates of non-fatal overdose remained high. As street drugs became increasingly toxic, interventions like Take Home Naloxone (THN) and Overdose Prevention and Supervised Consumption Sites (OPS/SCS) prevented nearly 6,000 deaths.
While public health used legal orders to make interventions like THN, OPS, and pharmaceutical alternatives to the toxic drug supply available, much of the immediate frontline response to the overdose emergency fell to communities of people with lived and living experience (PWLLE) of substance use and peer-run organizations which often operate services without sufficient and sustainable funding or organizational support.
“PWLLE are first responders. We’re the first people on the scene, who are there while it’s happening, who keep people alive until the government responders get there,” says Marnie Scow, who works with Professionals for the Ethical Engagement of Peers (PEEP) at the BCCDC.
As PWLLE respond to the overdose emergency, they are also directly affected by it. Many PWLLE face the reality of overdose risk themselves, and are exasperated by the overwhelming and continuous loss of family, friends, and loved ones.
Since BC declared COVID-19 a public health emergency, overdose deaths have reached an all-time high in the province. Visits to OPS/SCS have dropped since March, as sites closed temporarily or operated at reduced capacity to limit the spread of COVID-19.
At times, responses to the dual public health emergencies have been at odds. Although overdose deaths have consistently outpaced COVID-19 deaths (Figure 1), that’s not what one may expect, given the differences in media attention and scale of response between the two emergencies.
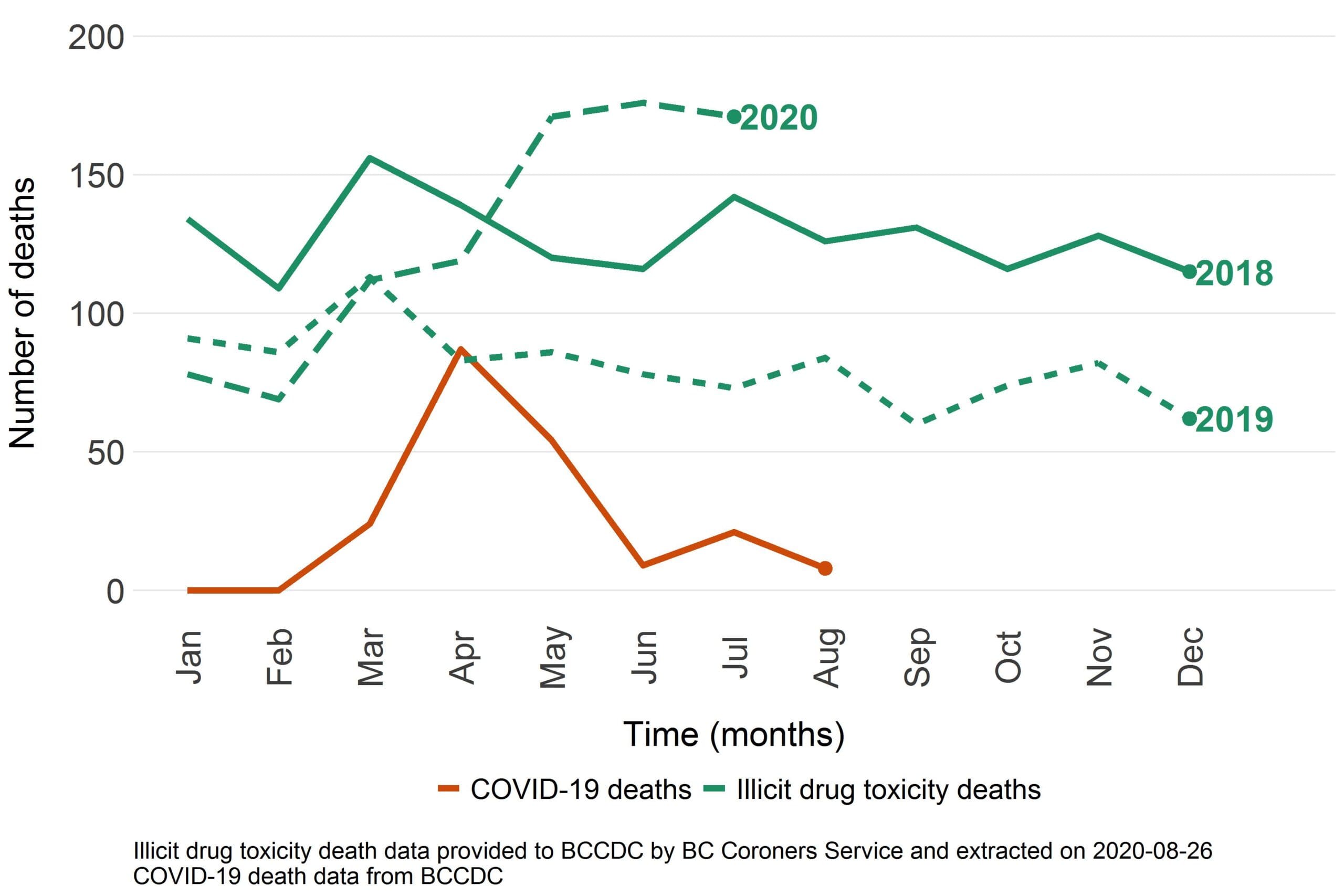
“I see the efforts and money that’s been put into COVID-19, and overdose has squashed COVID-19. It took COVID-19 for us to even get safe supply – it didn’t happen until lives besides drug users’ lives were at risk. It wasn’t enough that people were dying from overdose at alarming rates,” says Jenny McDougall of PEEP, speaking of Risk Mitigation Prescribing.
As of September, the Ministers of Health and Mental Health and Addictions have approved expanding access to prescribed pharmaceutical alternatives to the toxic drug supply: it no longer need reference COVID-19 prevention, and instead emphasizes the need to reduce reliance on an increasingly toxic drug supply.
While both emergencies have needed intervention from public health agencies, the nature of response that each requires differs greatly. Overdoses require medical intervention within minutes, and often happen in community settings or in housing.
Governments made use of the opportunity to scale up needed and cost-effective interventions for people who use drugs (PWUD). However, the fact remains that there was not enough political and social support to implement these interventions without COVID-19 prevention as a justification. This lack of political will reinforces stigmatizing messages from society.
“People who use substances have been criminalized to the point where no one cares about their lives,” says Paul Choisil of PEEP.
“The difference in scale of response sends us the message that lives of PWLLE are expendable—people who use drugs are not a priority,” Charlene Burmeister of PEEP added.
Provincial Health Officer Dr. Bonnie Henry’s position on the topic is clear: substance use in our society should be treated as health issue rather than a moral or criminal one. Chief Coroner Lisa Lapointe and the Canadian Association of Police Chiefs echo Dr. Henry’s sentiments.
PWLLE of substance use are moving society towards recognizing that caring for PWUD is an end in and of itself—it’s not just COVID-19 prevention. The Peer2Peer initiative at the BCCDC identifies and works to implement evidence-based interventions to support PWLLE responding to the overdose emergency.
As PWLLE put overdose prevention into action, and work to bridge the gap between communities and Health Authorities, they’re preventing overdose deaths and disproving stigmatizing beliefs about PWUD.
As Jess Lamb of PEEP stated, “We’re gonna do what we need to do to keep people alive.”
One of the initiatives led by the BCCDC, in partnership with the First Nations Health Authority, is Compassion, Inclusion, and Engagement (CIE). The BCCDC Foundation for Public Health has partnered to raise awareness and funds for CIE. Learn more about CIE and how you can support peers doing life-saving work.
Supplemental contributors:
Jenny McDougall
Regional Committee Member, Professionals for the Ethical Engagement of Peers (PEEP), BCCDC
Cheri Newman
Regional Committee Member, Professionals for the Ethical Engagement of Peers (PEEP), BCCDC
Jessica Lamb
Regional Committee Member, Professionals for the Ethical Engagement of Peers (PEEP), BCCDC
Paul Choisil
Regional Committee Member, Professionals for the Ethical Engagement of Peers (PEEP), BCCDC
Charlene Burmeister
PWLLE Stakeholder Engagement Lead, BCCDC
Marnie Scow
Regional Committee Member, Professionals for the Ethical Engagement of Peers (PEEP), BCCDC
Kurt Lock
Harm Reduction Program Staff, BCCDC
Connie Carter
Senior Policy Analyst, Overdose Emergency Response Centre, Ministry of Mental Health and Addictions
Carolyn Davison
Director, Overdose Evaluation & Monitoring, Overdose Emergency Response Centre, Ministry of Mental Health and Addictions
Margot Kuo
Senior Epidemiologist, Overdose Surveillance, BCCDC
Jane Buxton
Physician Epidemiologist & Medical Lead Harm Reduction, BCCDC



