“An ounce of prevention is worth a pound of cure.” Benjamin Franklin coined this phrase nearly 300 years ago about fire safety. Centuries on, it’s become the perfect motto for public health.
Prevention focuses on stopping harm before it occurs. When we prevent illness or injury we prevent pain and suffering; we promote positive health rather than focusing on cures or treatments only after harm has occurred.
The ‘ounce’ of prevention, therefore, is more valuable than the ‘pound’ of cure.
There are three general types of prevention:
- Primary prevention stops disease or injury before it occurs. The most well-known example of this in public health is vaccination.
- Secondary prevention reduces the impact of a disease or injury that has occurred, often through early detection. For example, breast cancer screening via mammography.
- Tertiary prevention focuses on management of existing diseases or injuries, and lessening the impact through certain measures. An example is prescribing insulin to manage diabetes.
Prevention is important in all aspects of our lives, and while we need to take care to prevent illness and injury for ourselves, we can also play a role in preventing illness, injury, and other problems on a population level.
Infectious disease, chronic diseases, racism, overdoses, and injuries: all preventable
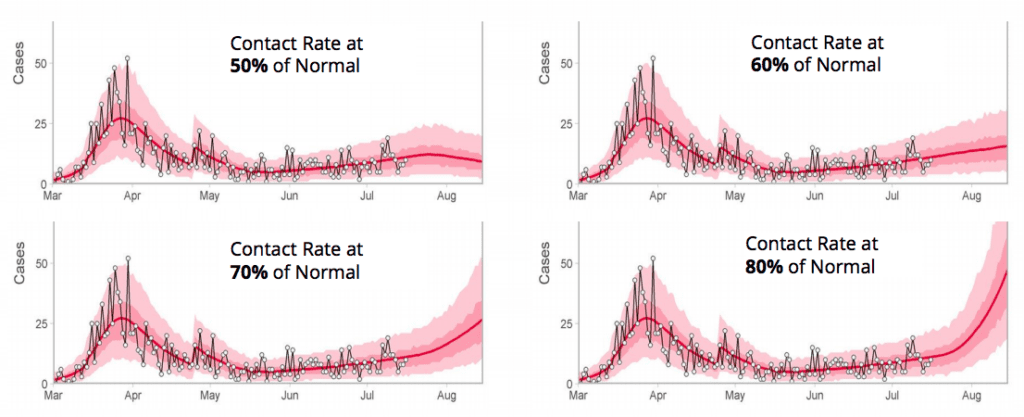
COVID-19 is an obvious example of why prevention is imperative to the health of our population. Infection prevention and control is the bedrock of public health, and we can see what happens when it’s done well. It works. In the case of COVID-19, it means we’re flattening the curve.
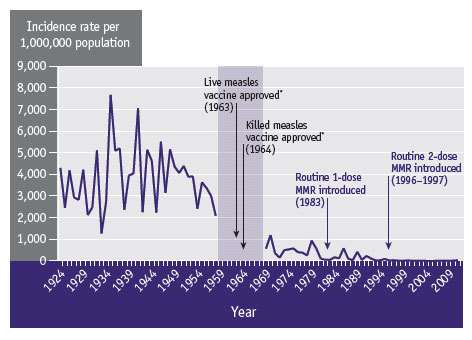
Immunization programs are an evidence-based solution to preventing disease. The advent of vaccines changed our world; they save lives every day. When immunization rates are sufficient we create herd immunity and the population is protected. Yet, when rates fall below appropriate levels (92-95% of the population for measles, for example), vaccine-preventable diseases can resurge, causing outbreaks that are completely avoidable. Vaccinations prevent disease. It’s that simple.
Research is showing we may be able to reduce asthma rates by reducing antibiotic use in infancy. Asthma is the most prevalent chronic childhood illness and hundreds of thousands of children in Canada struggle to breathe because of it. By taking upstream action, we can prevent these children and families from the fears, struggles, and risks that inherently comes with asthma.
We can prevent people from dying of drug overdoses by providing a clean and safer drug supply to combat the highly toxic illicit supply, and by eliminating the stigma associated with substance use.
We can prevent racism and the plethora of health inequities that come as a result of it, by breaking down and rebuilding systems, to dismantle the structures that have created and perpetuated systemic racism.
Most serious injuries are preventable, too. Read the blog post by Megan Oakey (Provincial Manager, Injury Prevention at the BCCDC) to learn more about injury prevention.
These are just a handful of examples that would have incredible outcomes for the health of our population if fully integrated into our society.
The common thread
There’s a thread that links everything we talk about—health equity, upstream action, the social determinants of health (SDOH), and social justice: health promotion. Through the principles of health promotion, we emphasize prevention and equity, we address the SDOH, and we create the healthy human. The human who requires less treatment and disease management, and fewer acute healthcare services, who lives in a supportive, safe, and positive environment, driven by healthy public policy, and is enabled to take control of their own health and well-being.
Change can start with us
All this sounds pretty important, doesn’t it? It is. Yet, it isn’t prioritized it in our healthcare system. If an ounce of prevention is worth a pound of cure, why don’t we invest more in prevention and health promotion? Because seeing population- and system-level impact takes longer, and we all too often value the quick response, the instant gratification, the individually-focused model. By investing in prevention, we will reduce the burden on our healthcare system, and will ultimately be able to shift resources to provide a more holistic system of ‘care’.
We can use our individual actions and voices to move towards a new way of thinking:
• Support and advocate for an enhanced role for prevention in our healthcare systems, in our social safety nets, and in our schools and communities.
• Prevent COVID-19 by following public health recommendations.
• Get vaccinated, and stay up-to-date with boosters and immunizations needed for adults.
• Demand government invest in upstream solutions to end the overdose crisis, and reallocate resources to support positive mental health solutions.
• Stop stigma; call out systemic racism.
Shifting our mindset, system, and resources requires a collective commitment.
